June 1, 2015 – Ottawa, ON – Public Health Agency of Canada
Today, the Chief Public Health Officer of Canada Dr. Gregory Taylor launched a consultation process to support the development of a Federal Framework on Lyme Disease.
This consultation will solicit perspectives on Lyme disease from the medical community, governments, patients’ groups, as well as individual Canadians.
Specific feedback will be solicited on three key themes of the Federal Framework, as outlined in the Act:
- National medical surveillance: to track incidence rates and the associated economic costs of Lyme disease in Canada.
- Guidelines and best practices: the prevention, identification, treatment and management of Lyme disease and sharing of best practices throughout Canada.
- Education and awareness: to develop standardized educational materials for use by Canadian public health providers to increase national awareness about the disease.
The Public Health Agency of Canada’s current Action Plan on Lyme Disease will serve as a platform for the development of the Federal Framework. It aims to mitigate the risks to Canadians posed by Lyme disease through three pillars: engagement, education and awareness; surveillance, prevention and control; and research and diagnosis.
Stakeholders and the public are invited to participate in the online consultation. Comments will be accepted until June 30, 2015.
A Conference will be held with invited stakeholders later this year where the input received through the consultation will inform the development of the Framework.
Blog
Tick PSA From Flo Gardipee ~ Wildlife Biologist with Lyme

Via Flo Gardipee (friend and fellow Wildlife Biologist with Lyme):
To all my friends & family, especially fellow biologists and park rangers, that spend time in the outdoors, please take precautions against tick bites. If you find a tick attached to you, remove it and save it to send in for testing, then get to a Dr right away for treatment with antibiotics. Ticks carry awful diseases such as Lyme, Bartonella, Babesia, Erlichia, Rocky Mtn spotted fever, and others.
Continue reading Tick PSA From Flo Gardipee ~ Wildlife Biologist with Lyme
My story in Hungry Horse News ‘Ticks: One woman’s warning’

“My daughter knows what I was like before I was sick,” she said with tears in her eyes. “My son doesn’t.”
Ticks: One woman’s warning
By CHRIS PETERSON Hungry Horse News, May 27, 2015
In April 2010, Angela Daenzer was doing field work as a biologist for the Flathead National Forest when she startled a moose up the Middle Fork. She ducked off into the brush to avoid the angry animal, and while the moose encounter was a bit scary, there were worse things to come.
While hiding in the brush, Daenzer picked up a tick that bit her in the scalp. After a shower hours later, she found the tick and, disgusted by it, she pulled it out of her hair and threw it in the toilet.
Daenzer is convinced that tick gave her Lyme disease, or at the very least a disease very similar to it. Within a week, she became very ill. She got the chills and a sore throat and then what she and her doctors thought was an ear infection and then severe jaw pain.
How CDC Lyme Disease Surveillance Maps Can Keep You Sick
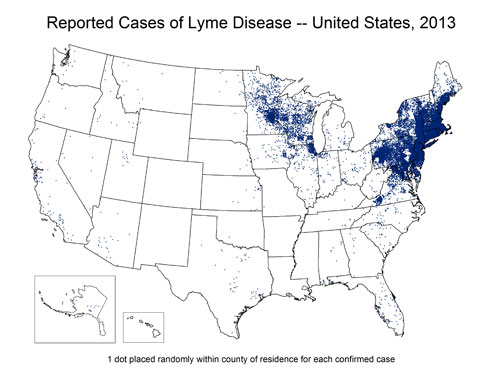
The spatial display of non-spatial or improperly represented Lyme disease data is endangering patients and misleading doctors, with life-altering, expensive, debilitating, and potentially fatal consequences. This is especially true in regions (such as the Northern Rockies) where detection effort is reduced by the very biases and presuppositions most of these maps create.
CDC Lyme Surveillance Maps do not represent where cases are contracted but are used and/or interpreted as depicting the geographic distribution of the illness. The act of placing the dots on a map implies a geographic relationship with the information being displayed….if the relationship intended is supposed to be diagnosis locations only (which these dots currently represent), this should be the title of the map, rather than a fairly minor foot note.
Continue reading How CDC Lyme Disease Surveillance Maps Can Keep You Sick
Times Colonist Article Link ~ Speculation Regarding Lyme In Canadian Rockies
Monique Keiran: Tiny ticks a good reason to be cautious
May 24, 2015
My former (and now future) anti-tick precautions predate confirmation that ticks in western Canada carried the dreaded Borrelia bacteria. Instead, I grew up on tales of Rocky Mountain spotted fever, tick paralysis and other ailments shared by the seed-sized critters. It was only during my last few years in the mountains that Lyme disease loomed locally as a possibility.
I recently met a colleague from those mountain days. He mentioned that several people he had worked with in the 1980s now suffered from unaccounted-for neurological problems, including memory loss, chronic fatigue, muscle wasting and nerve issues.
He speculated about Lyme disease, but didn’t know. He said the acquaintances also didn’t know. Three decades have passed since they spent their summers roaming slopes, exploring valleys and camping in high-mountain passes.
Lyme disease might have existed in the Rockies back then, but remained undetected, undocumented and unknown. The bacteria can incubate for years in some people before causing illness. It’s also possible the illness occurred back then, but lack of awareness and difficulties with diagnosis — which continue today — left it undiagnosed.
– See more at: http://www.timescolonist.com/opinion/columnists/monique-keiran-tiny-ticks-a-good-reason-to-be-cautious-1.1944790#sthash.fuhfwAYX.dpuf
Related link and additional future links posted HERE.
FCCLA Lyme Disease Challenge Booth at Columbia Falls High School Tomorrow!

I’m so proud of my daughter for this idea and grateful to the leadership club for making it happen. They will have a booth with facts and limes ready for any students that want to do the challenge.
You can read more about the challenge at LymeDiseaseChallenge.org and LIKE THEIR FACEBOOK PAGE ~ HERE~. You can also see my daughter’s earlier challenge videos, my son’s videos, and featured regional challenges (so far) on our Regional Challenges Page (including a link to our challenge to Ride For Lyme, which they have accepted).
A high school teacher and junior high teacher were instrumental to my diagnosis, and I finally caught up with one of them by letting them know about the booth (having not spoken since my diagnosis). There’s a slight chance I may meet her in person (for the first time) one of the days of the booth, but we will definitely have to meet soon.
Stay tuned for more from this proud mom.

Which Borrelia Strains Are We Contracting in the Rockies?

As is often the case with Lyme-related questions in this region, this question has two important parts. One being which are we contracting within this geographic area, and the other being which are we contracting anywhere else that we travel to?
It’s challenging, but important, to distinguish the relative importance of each part of the question. As a patient in a time-sensitive quandary, it doesn’t matter where we contracted the illness as much as it matters that we can get timely and adequate diagnosis and care. But a current obstacle to both in this region, unfortunately, is the assumption that contracting it here is not possible, because it serves as a very large distraction and obstacle, regardless of where the exposure occurred.
 The fact that you ‘can’t get it here’ is, sadly, often the only answer the patient receives–an untimely and unjustified end to what should be a lengthy discussion including a number of important questions.
The fact that you ‘can’t get it here’ is, sadly, often the only answer the patient receives–an untimely and unjustified end to what should be a lengthy discussion including a number of important questions.
This is a problem, of course, because we need medical care either way, and it needs to occur quickly to avoid the risk of permanent harm to the patient.
So the importance of proving we can contract Lyme in the Rockies is partly to overcome the wrong assumption that it is not a risk here, but also to overcome the biases among doctors that lessen the chances of due consideration of the likely cause of symptoms that present ‘just like Lyme disease’ but ‘can’t be Lyme disease’ (in most cases until the patient is able to travel out of state for a more informed opinion*, which is usually not happening fast enough to avoid long term consequences).
Continue reading Which Borrelia Strains Are We Contracting in the Rockies?
Alberta ~ Results of Tick Submissions by Veterinarians ~ From Jill McAllister

This graphic by Jill McAllister is extremely meaningful, as it provides information not currently available in terms of geographic distribution of Lyme and Lyme infected ticks.
Some of these locations, although across the border, are not really all the far from where I was bit in 2010 (various maps will be constructed over time). As you will read elsewhere on this site, distribution estimates and maps can be dangerously misleading if they do not depict associated levels of detection effort. As is seen time and time again (with North Dakota serving as a highly relevant example) the areas where we are not finding Lyme coincide with areas where we are not yet, or not adequately looking.
Ride For Lyme ~ You Have Been Lyme Disease Challenged!

Our very first collective Lyme Disease Challenge goes out to Dan and Tanner and the Ride for Lyme team (aka the Adalaine project), in a location of their choosing as they cross the continent for Lyme patients and their friend!
This challenge includes the patient they ride for that day, IF the patient is well enough. If not, we’ve got that patient covered, as we’ll be doing extra ‘bites’ on behalf of that patient in their honor.
So, Dan and Tanner, here’s how the Lyme Disease Challenge works!
Continue reading Ride For Lyme ~ You Have Been Lyme Disease Challenged!
Dear CDC and FDA ~ By Melissa VeHorn
Posted with permission. This is not from the Northern Rockies, but clearly applicable to all of us. Thank you Melissa.
Dear CDC and FDA,
I don’t want to just go away.
I want to live!
I have a lot to offer this world.
I am not just a number or face in a massive population.
I am a mother, daughter, wife, sister, aunt, friend who has a giving heart and creative mind.
Please.
My life matters.
I am here for such a time as this.